— by Sarah Ladd, Kentucky Lantern —
This article mentions suicide. The number for the National Suicide Prevention Lifeline is 988.
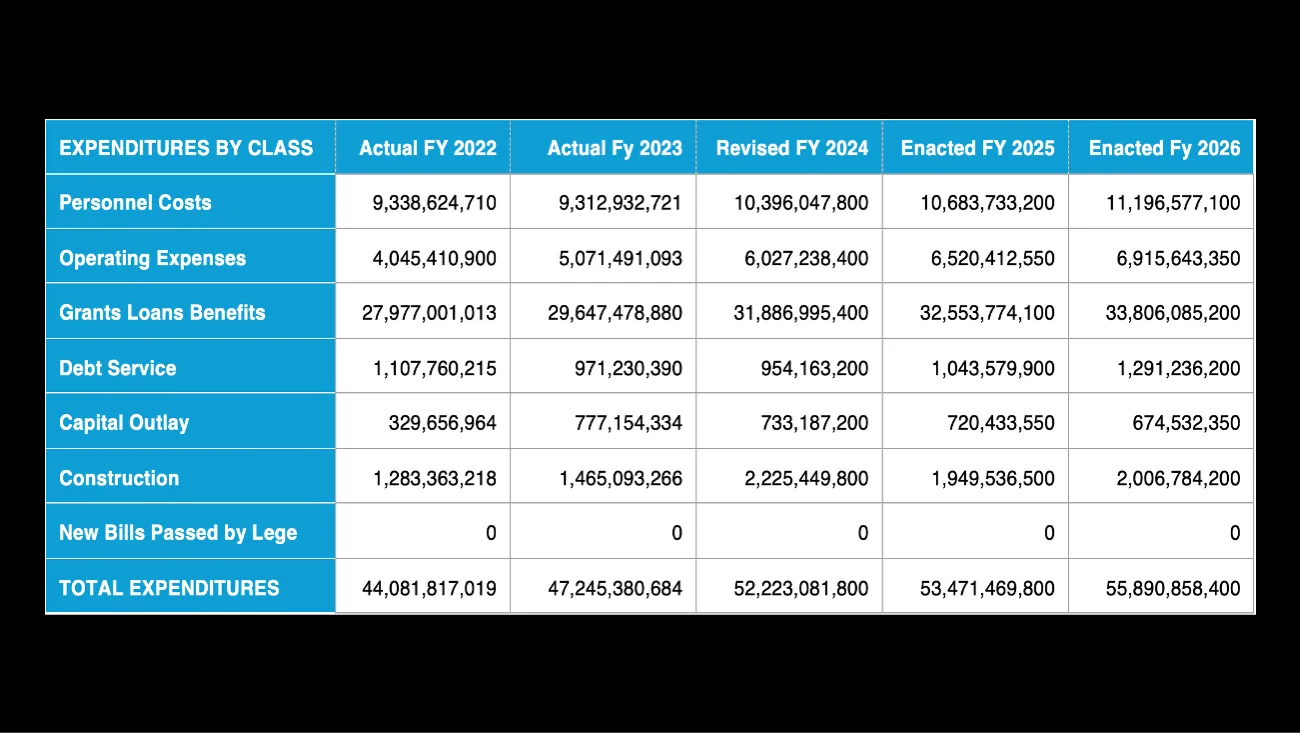
Changes the Kentucky General Assembly ordered in Medicaid face an uncertain future after Gov. Andy Beshear said lawmakers failed to fund the legislation.
For the second year in a row, Beshear last week sent the House and Senate a letter listing bills that they had passed without providing what Beshear said was the necessary funding.
Beshear sent the letter on the next to last day of the 2025 session, listing 11 bills and writing “there is still time in this legislative session to add appropriations.”
The Republican-controlled legislature took no action in response to the Democratic governor’s letter, and Senate President Robert Stivers (R-Manchester) told reporters Beshear is obligated to carry out laws as enacted by the legislature.
“He wants to make some excuse about, ‘oh, you didn’t give me the money.’ But it’s basically: ‘yes, you do have the money. Find it within your budgets,’” Stivers said.
Among the 11 bills that Beshear said lack “the appropriations necessary to implement” them is House Bill 695, which directs the Beshear administration to take steps to enact a Medicaid work requirement while prohibiting the administration from making any changes in the $15 billion program without first receiving the legislature’s approval. The bill also creates a Medicaid Oversight and Advisory Board to look for cost savings in Medicaid.
Beshear vetoed the bill and the legislature easily overrode his veto.
The clash comes as Democrats in Washington are bracing to fight Republican efforts in Congress to cut Medicaid — a federal-state program that covers health care for low-income people — in order to pay for renewing federal tax cuts.
In the letter, Beshear said HB 695 would require rebidding Medicaid managed care contracts, which he said would cost the state $1.4 million, including hiring a contractor to help develop the request for proposal. The bill also is estimated to cost $500,000 in state funds to conduct a managed care long-term service study, Beshear wrote.
In his veto of HB 695, Beshear said the Medicaid community engagement requirement, commonly called a work requirement, would “undoubtedly” cost some adults their health coverage and also spark costly litigation challenging the requirement.
Emily Beauregard, the executive director of Kentucky Voices for Health, said health care advocates are concerned about new costs associated with a work requirement. “One of our concerns all along with HB 695 has been the additional administrative cost it requires to ultimately provide less health care, which isn’t a good use of taxpayer dollars,” she said.
Beshear’s letter to lawmakers last week echoed one he sent the year before, which has sparked a lingering controversy over the state’s failure to fund relief for kinship care families.
Lawmakers have previously said Beshear has misinterpreted a 2005 state Supreme Court decision that he says precludes the executive branch from spending money the legislature has not appropriated. That decision came out of a cycle when the General Assembly passed no budget.
Still, Beshear wrote: “These holdings are simple: if the legislature creates a policy or program but does not provide funding, it does not intend for the executive branch to perform those services over the biennium. The omission of an appropriation is the same as its elimination.”
Beshear also cited a more recent federal court decision.
On Friday, Stivers criticized Beshear’s handling of the kinship care issue, which resulted in months of back and forth with no solution for families who are raising minor relatives and need more assistance.
“He decided to expand Medicaid rolls, not do kinship care, but then he says he doesn’t have the money to do it,” Stivers said. “He picks and chooses what he wants to do, even though we’ve told him what to do.”
“We’ve talked about on this floor all the things he decided to fund without authority, things he does without authority. We send him bills, and it’s his obligation to carry out those laws that we change and empower him to execute on,” Stivers said.
Most of the funding for Medicaid comes from the federal government. Beshear said 1.6 million Kentuckians are covered by Medicaid and the Children’s Health Insurance Program.
Beshear’s letter to lawmakers also said they had failed to take into account the costs of their decision to protect conversion therapy. House Bill 495 overrules restrictions Beshear had placed on the discredited practice and also prohibits Medicaid from covering transgender-affirming medical care. Beshear estimated it would cost $540,000 to $1.95 million in state funds.
“Other states with similar laws have experienced an increase in suicide attempts, some by as much as 72%,” Beshear wrote. “The increase in services expected include an additional six hours of behavioral health counseling and therapy, an increase in pharmacy costs and increased psychiatric hospitalization.”
Among other bills Beshear said the legislature failed to fund:
- Senate Bill 4, which he said would cost at least an estimated $2.5 million to operate a centralized registry of artificial intelligence systems in state government and implement an AI governance process.
- House Bill 390 to set up an accessible online vehicle insurance verification system, which Beshear said would cost $600,000 to $1.1 million initially and then $750,000 a year to operate.
- Beshear also said that House Bill 346, exempting emergency temporary internal combustion engines from paying an emissions assessment fee and to retroactively refund some fees, would cost the Division of Air Quality $1 million in expected revenue from fees.
--30--
Written by Sarah Ladd. Cross-posted from the Kentucky Lantern.